Periodontal Disease
The last five years have shown that periodontal health can have a major impact on a patient’s general and systemic health. A chronic bacterial infection, periodontal disease can lead to a higher incidence of bacteria in the bloodstream, circulating to various organs of the body. These bacteria can then bind with blood platelets and cause an increase in clot formation in arteries and tissues. Those with periodontal disease have a higher risk factor with the following diseases.
Periodontal disease occurs when an infection of the gum and/or bone surrounds the tooth. Because this disease can be painless, most patients are not aware that they have a problem until examined by a dentist. With a healthy tooth, the root is formed in the jawbone with a strong ligament. This keeps the tooth tightly attached to the bone. Gum protects the bone from bacterial constantly present in the mouth. When healthy, the gum edge is higher than the fiber attachment. In turn, a space is formed around the tooth. This mirrors having a turtleneck sweater.
We all have bacteria in our saliva continuously. Yet, when these bacteria collect on all surfaces, plaque forms. If the plaque in the space underneath the gum edge is not removed, infection may occur. The longer that plaque remains on a tooth, the more problems it can cause. Once it hardens, it becomes what’s known as tartar and must be dislodged by a dental professional.
Stage 1 of Periodontal disease
At first, patients experience gum inflammation or gingivitis. As cells are carried to destroy the bacteria, the gum tissue appears red and swollen. Sometimes this may lead to bleeding when the teeth are being brushed.
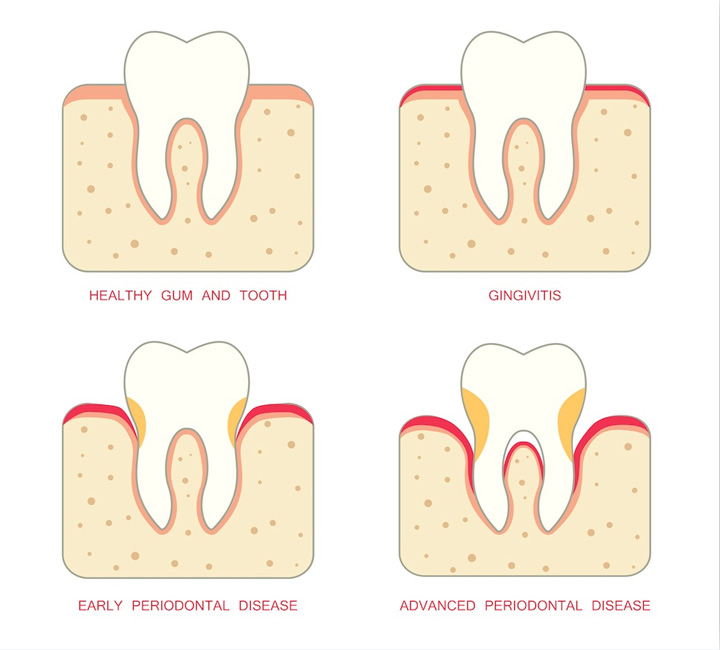
Stage 2 of Periodontal disease
Bone destruction around teeth has not occurred yet, meaning regular brushing and flossing should correct the problem. If not corrected, the bacteria may destroy the fiber barrier and move down the surface of the tooth. Inside lining of the gums and bone are consequently destroyed. A deepened space between the gum and tooth, called a periodontal pocket, is created from the penetration of bacteria. Using a periodontal probe, your dentist can measure the amount of bone loss that has occurred. Bone loss yields a major weakening in tooth support. Eventually, the tooth becomes loose and falls out if the disease goes untreated.
Periodontal Disease Treatment
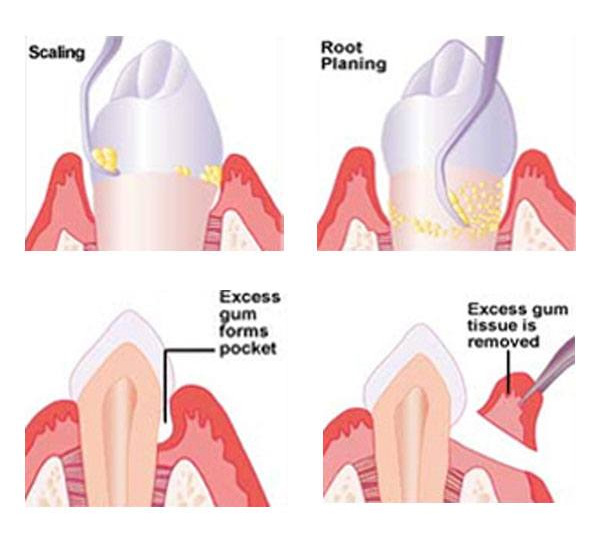
Initially, the pocket depth of the affected gum is typically only slightly deepened. To remove any calculus that has formed, scaling and root planing are done. In order to prevent discomfort, we may numb the gums to protect the tender pockets. It is necessary patients maintain good oral habits following the procedure to keep plaque from reforming. Your oral health will return as soon as the healing gum builds back up around the tooth.
Swollen gums that fail to shrink back to normal must be corrected with a gingivectomy. Patients will experience the same issue if this procedure is not performed.
Actual bone loss takes place in more moderate cases, where the pockets are 5-7 mm in depth. Flap surgery is usually the procedure needed because of the difficulty in reaching the bottom of the pocket with scaling and root planing. Flap surgery involves an incision made between the gum and tooth. The gum is peeled back away from the neck of the tooth and bone edge. This enables the surgeon to easily see the deep calculus and properly debride the tooth.
An successful flap surgery results when the periodontist surgically removes the pocket by repositioning the gum down to the new bone level. The surgeon first corrects any irregularities or pitting of the bone and the gum is sutured down to the re-contoured bone. Patients are able to remove the bacterial plaque with brushing and flossing once the pocket is eliminated. As long as patients abide by this daily, the disease is stopped.
Diagnosis And Treatment Of Periodontal Disease
- Diagnosis
- Clinical Examination
- X-Rays
- Diagnosis
- Treatment
A proper diagnosis involves a review of the patient’s medical history, clinical examination and x-rays. This allows us to have a better understanding about the disease’s progression rate and enables the surgeon to determine what needs to be done to avoid further breakdown.
Completing a medical history will point us to whether a patient has certain risk factors, resulting in a modified treatment. Below are the most significant general health considerations that may affect susceptibility to periodontal disease.
Periodontal Maintenance and Follow Up Care
Good periodontal health is maintained with good oral hygiene and regular dental cleanings. Research proves that those who fail to maintain quality dental habits have 20 times the amount of bone loss as those who do.
To prevent reoccurrence of periodontal disease, it is essential that patients remove plaque twice daily. Maintaining good dental habits and regular cleanings are critical to long-term oral health. With inadequate follow-up care, the disease will come back. That’s why the patient must take full responsibility for their periodontal health.
In cases where residual pockets are deeper than 3 mm, or where the patient has exhibited a high susceptibility to breakdown, it is critical that we perform three-month recalls. This is done to manage the bacteria from forming plaque immediately after treatment. Read more
Plaque usually takes about three months to develop into an aggressive infection. While minimal bone loss takes place within the first three months, the likelihood of breakdown dramatically increases after 90 days. The aggressiveness of plaque will be kept to a minimum as long as plaque is regularly removed.
The two essentials of oral hygiene are brushing and flossing. Patients should slide the bristles of the brush into the cuff of the gum, like a broom may slide under the edge of the refrigerator. Positioned at a 45 degree angle to the tooth, move the brush in a circular motion. This method is the best way to remove plaque from beneath the gum edge. We do not recommend a scrubbing motion, as this may lead to gum recession.
Please be aware of the following procedures performed at the periodontal maintenance appointment.
- Update of dental and medical history
- Soft tissue cancer exam
- Clinical decay examination
- Clinical periodontal examination
- Review of proper oral hygiene as needed
- Scaling above gum level
- Root planing under gum level
- Polishing
Every three months, we take full mouth radiographs to determine the stability of the bone level.
A key observation at the appointment will be whether there was bleeding when performing probing of the tissues. No bleeding leads to a healthy mouth. Additional treatment will be warranted if bleeding does exist. We will also take note if the x-rays show a change of bone level. Throughout the periodontal maintenance appointment, we want to make sure that patients are comfortable. We have nitrous oxide available for those who need help relaxing
